The Short Answer: Yes – But It Is More Complex Than You Think
If you have erectile dysfunction (ED), stress, poor sleep, or anxiety, they can make things worse. Your body’s stress response may impact your sexual performance. A key factor in this connection is a hormone called cortisol, often referred to as the stress hormone.
High cortisol levels can result from long-term stress, Cushing’s Syndrome, or certain medications. ED links to these levels. Studies from top medical journals show that cortisol can disrupt several body systems. These systems are crucial for healthy sexual function.
That said, the connection is not straightforward. Cortisol does not always cause ED directly. It can also lower testosterone levels. This disrupts nitric oxide activity and affects blood flow. It increases nervous system tension and can trigger stress-related anxiety.
Understanding cortisol’s role in ED requires a clearer view of both physical and psychological factors. This is due to their overlapping effects.

Key Clinical Facts: Cortisol and Erectile Dysfunction
Higher cortisol levels are connected to lower scores in erectile function. This is based on clinical tests of blood and saliva. Men with ED often have high baseline cortisol levels. Their cortisol may not lower as it should during sexual activity.
In Cushing’s Syndrome, many men experience lower libido and trouble with erections. Cortisol levels usually fall during arousal, which helps blood flow. However, in some people, this response might not work well.
Men with stress-related ED might have high cortisol levels, even during intimate times.Lower testosterone levels have been observed in individuals with chronically high cortisol.
Chronic stress from obesity, diabetes, depression, or alcohol use can strain the stress response system. This increases the risk of erectile dysfunction (ED).
What Is Cortisol? Understanding the Stress Hormone
Cortisol is a hormone released by the body in response to stress. High levels of this substance are key to energy, metabolism, and immune health. High levels can disrupt normal body functions, including sexual health.
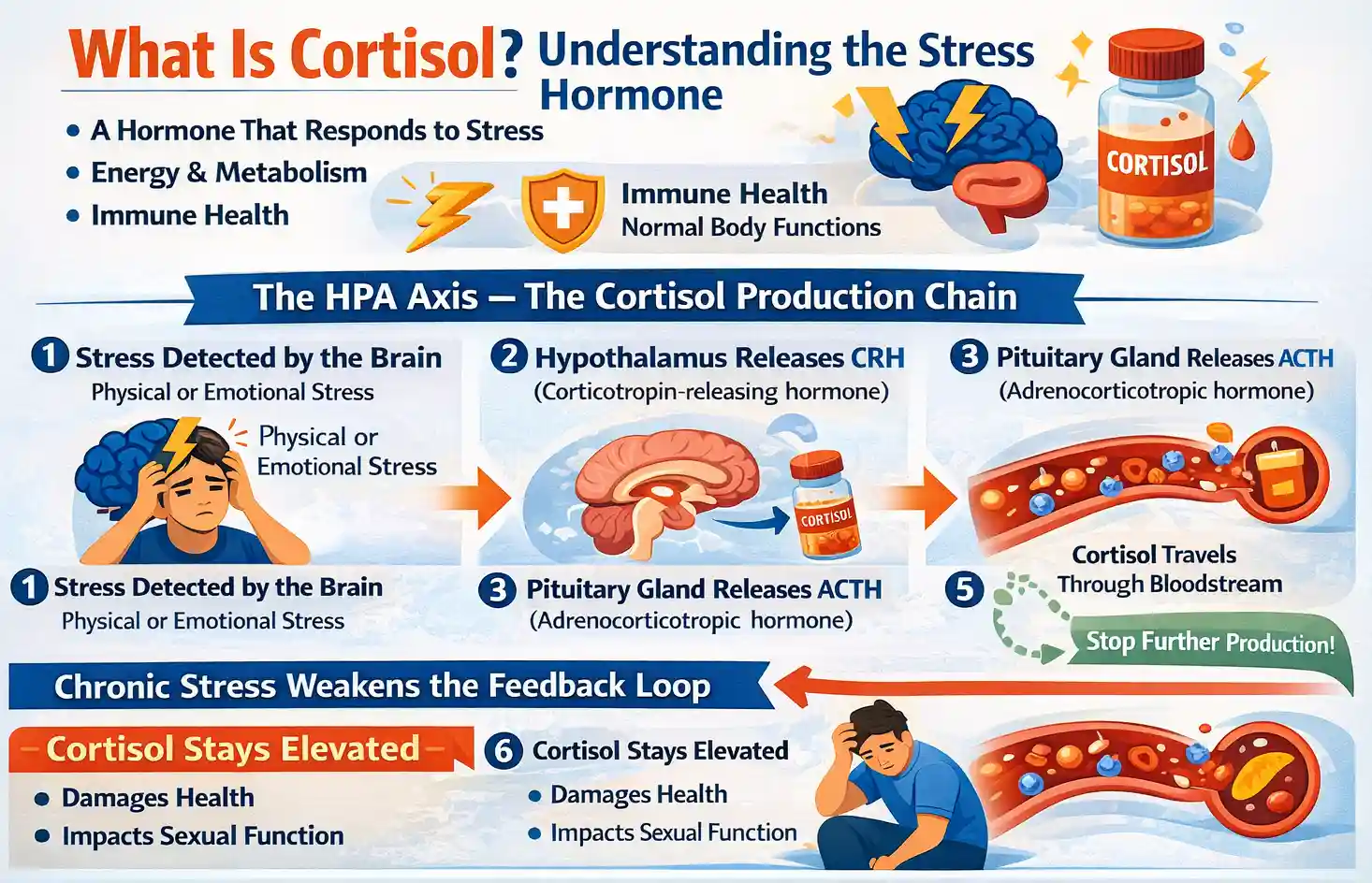
The HPA Axis – The Cortisol Production Chain
The body controls cortisol using the HPA axis (Hypothalamic-Pituitary-Adrenal axis). This system works like a communication chain between the brain and the adrenal glands.
What goes wrong?
Chronic stress makes this feedback system weaker. As a result, cortisol levels stay high. This can harm health, including sexual function.
How High Cortisol Causes Erectile Dysfunction – The 5 Pathways
Pathway 1: Cortisol Lowers Testosterone (HPG Axis Disruption)
Cortisol impacts erectile dysfunction by disrupting the HPG axis. This axis is key for regulating testosterone production.It reduces the release of GnRH (gonadotropin-releasing hormone) from the hypothalamus.
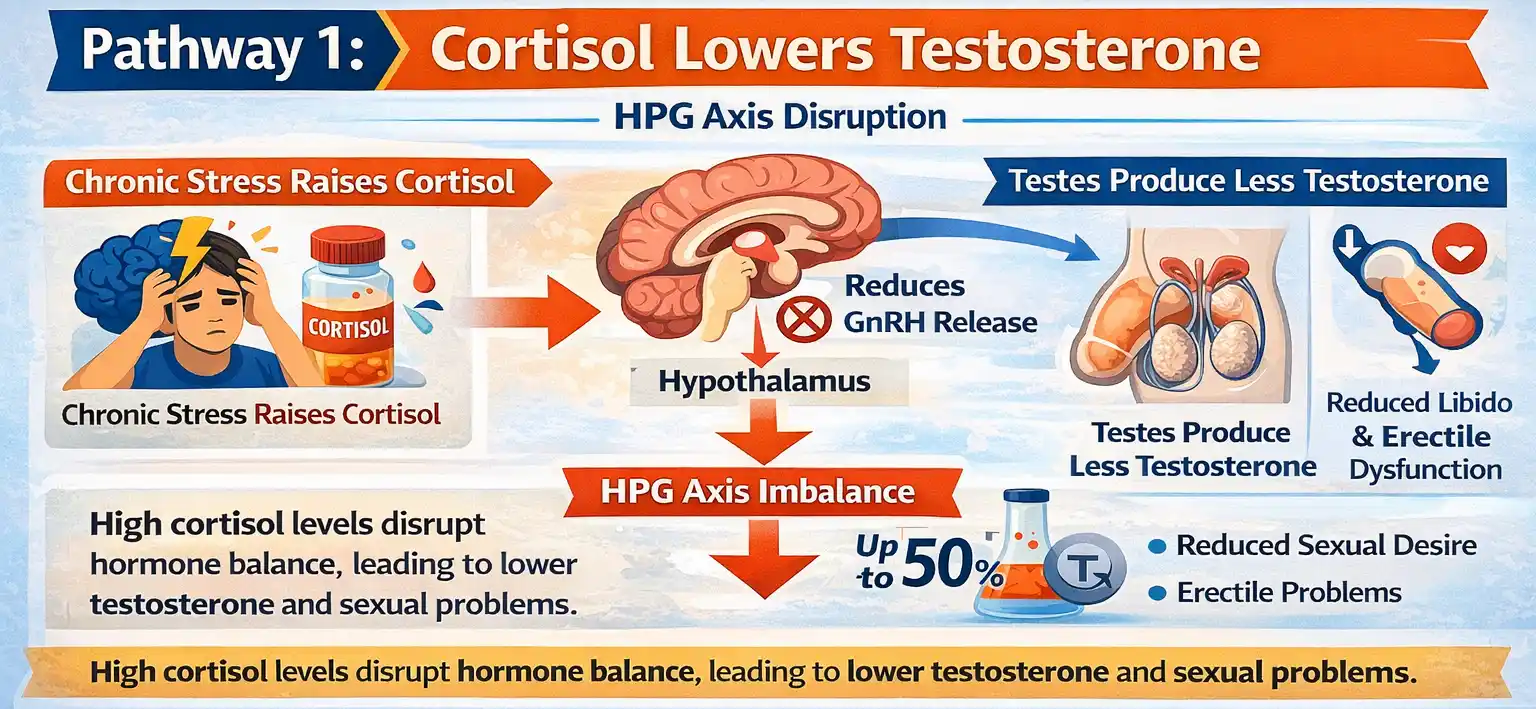
The testes make less testosterone. This hormone is important for sexual function. Lower testosterone is often one of the earliest signs of prolonged stress and plays a key role in reduced libido and weaker erections.
Men with high cortisol levels, like those with Cushing’s Syndrome, often have lower testosterone. This drop can exceed 50%.
They may also face reduced sexual desire and higher rates of erectile dysfunction. High cortisol disrupts hormone balance. It lowers testosterone, which affects sexual performance and reproductive health.
Pathway 2: Cortisol Disrupts Nitric Oxide (NO) Signaling – The Key to Erections
Nitric oxide (NO) is key to getting and keeping an erection. However, cortisol, known as the stress hormone, disrupts this process.
During sexual stimulation, specific nerve signals in the penis trigger the release of nitric oxide. This molecule turns on an enzyme named guanylate cyclase.
This action boosts levels of cyclic GMP (cGMP). Increased cGMP relaxes smooth muscles in the corpus cavernosum. This relaxes the erectile tissue and lets blood flow into the penis, creating an erection. Sildenafil and tadalafil help by stopping the breakdown of cGMP. This keeps the muscles relaxed longer and boosts blood flow.
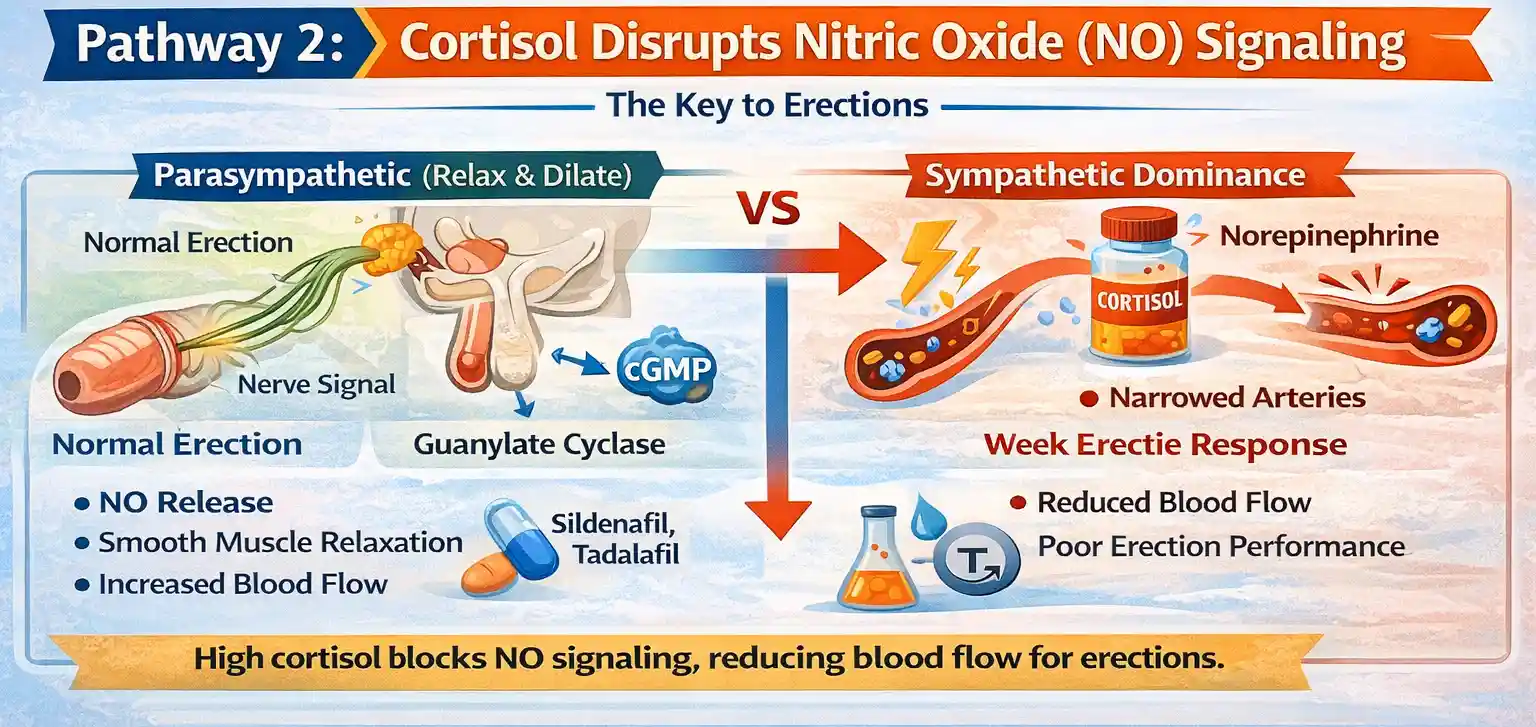
However, chronic stress and elevated cortisol levels disrupt this pathway. High cortisol triggers the body’s sympathetic nervous system, or “fight-or-flight” response.
This results in the release of norepinephrine. This chemical makes blood vessels tighten. This counters the vasodilation needed for erections. Nitric oxide signaling weakens. This lowers blood flow and harms erectile function.
Erection relies on relaxation and increased blood flow, driven by parasympathetic activity. Cortisol causes tension and reduces blood flow.
This happens because of sympathetic dominance. High cortisol levels over time keep the body stressed. This blocks what is needed for a healthy erection.
Pathway 3: Cortisol Drops During Healthy Erections – But NOT in Men With Psychogenic ED
In normal sexual function, cortisol levels naturally decline during arousal and erection. This drop happens in the bloodstream and in the penile tissue.
This shows that reducing stress hormone activity is key for an erection to occur. The body moves from stress to relaxation. This helps blood vessels open up and improves blood flow.
In men with psychogenic (stress-related) ED, cortisol levels do not drop. Cortisol levels stay high even during sexual stimulation.

This stops the body from getting into the relaxed state needed for an erection. This issue is not just psychological; it has a clear biological basis linked to hormone regulation.
Successful erections depend on two key factors: activating pathways that help erections and reducing stress responses. When cortisol does not decrease, the body remains in stress mode. This directly affects normal erectile function.
Pathway 4: Cortisol Causes Vasoconstriction – Reducing Blood Flow to the Penis
An erection happens when blood quickly fills the penis. This occurs through special arteries that must widen to let more blood flow in. Blocked blood flow or non-expanding blood vessels make it hard to get or keep an erection.
Cortisol disrupts this process by activating the body’s stress-response system. This triggers the release of chemicals like norepinephrine.
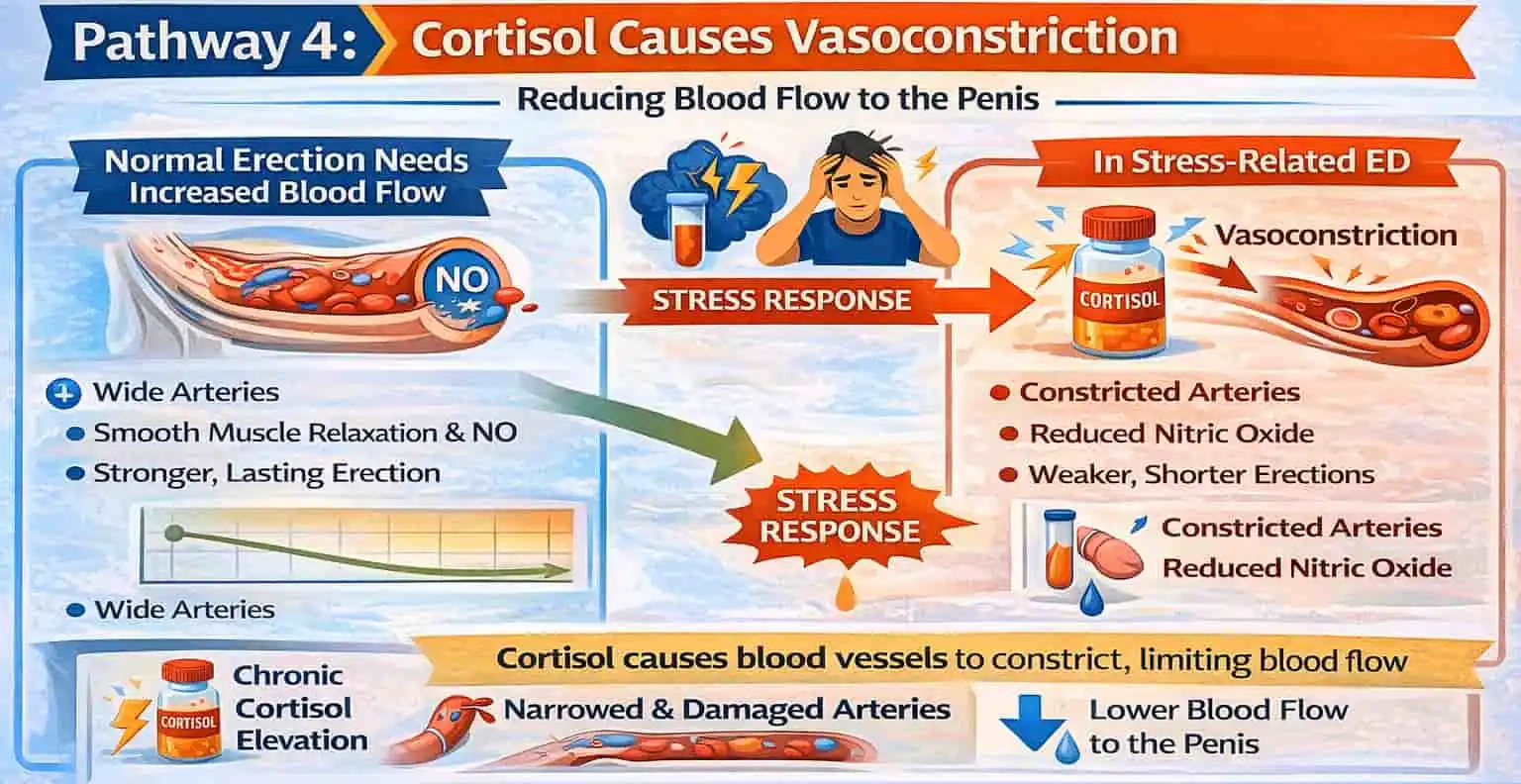
These chemicals cause blood vessels to tighten, or vasoconstrict, instead of relaxing. High cortisol levels can harm the endothelium, the inner lining of blood vessels. This damage reduces their ability to make nitric oxide, which helps relax the vessels.
Reduced nitric oxide and narrowed blood vessels limit blood flow to the penis. This results in weaker or shorter erections. Long-term stress hormones can harm vascular health. This issue worsens with conditions like diabetes, obesity, or depression.
Chronic cortisol elevation narrows blood vessels and harms circulation. This directly opposes the blood flow needed for a normal erection.
Pathway 5: The Psychological Feedback Loop – Cortisol, Anxiety, and Performance Pressure
The Cortisol-ED Anxiety Cycle
Stress, anxiety, and cortisol can form a cycle that worsens erectile dysfunction over time.
Chronic stress starts the cycle. It raises cortisol levels, making it hard to get an erection at first. After this first experience, many men develop anxiety and a fear of repeated failure. This psychological pressure then triggers even more cortisol release during future sexual situations.
When cortisol rises, it disrupts key erection processes. It reduces nitric oxide activity, lowers testosterone, and restricts blood flow. A failed attempt raises anxiety and keeps the problem going.
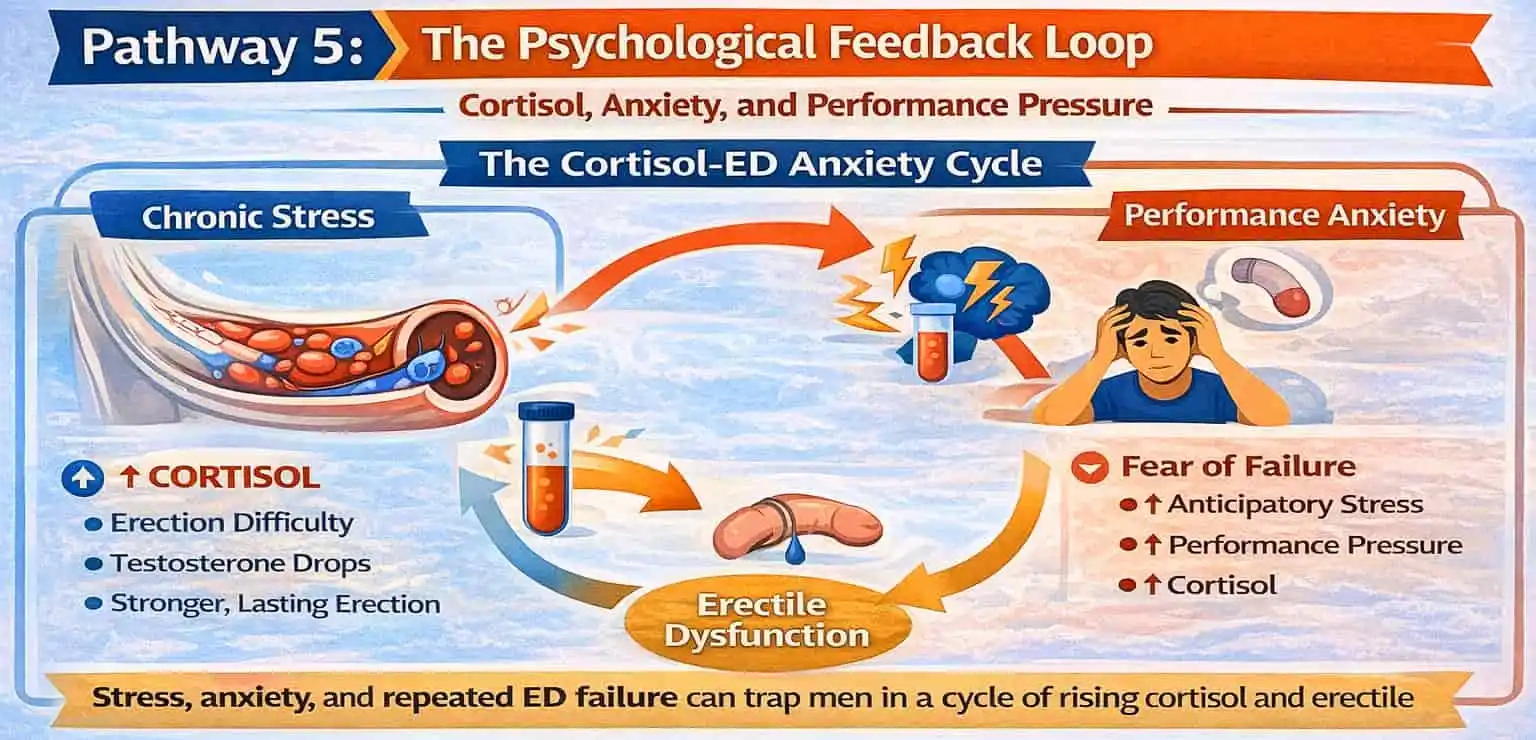
Over time, the brain links intimacy with stress instead of relaxation. This causes cortisol levels to rise even before sexual activity starts.
This ongoing loop means that even if the original stress is gone, the pattern can continue. The body has learned to respond with anxiety and higher cortisol levels.
Medications that just improve blood flow may not fix the problem. They do not tackle the stress-hormone cycle underneath.
Who Is Most at Risk?
Some men are more prone to stress-related hormonal imbalances; this can lead to erectile dysfunction.Men aged 35-60 dealing with long-term work pressure or financial stress.
Sleeping less than 7 hours a night can quickly lower testosterone levels. This often happens because of poor sleep habits. Men suffering from anxiety disorders, where chronic stress can impact sexual performance
Overweight or obese men, especially those with belly fat, often have hormonal imbalances. They also see reduced blood flow. People with diabetes, depression, or alcohol dependence may have a strong stress response system. This system is known as the HPA axis.
Symptoms – Is Your ED Cortisol-Driven?
To see if stress and cortisol are causing ED, look for both physical and sexual patterns.
Physical Signs
Gradual loss of morning erections, which are usually a sign of healthy hormonal function. Reduced sexual desire even when attraction to a partner is present. Constant fatigue, low energy, brain fog, or mood changes.Increase in belly fat, as high cortisol promotes fat storage around the abdomen
Sexual Signs
Erectile issues that worsen during periods of stress or emotional pressure.Struggling to maintain an erection during sex with a partner is common. This issue is often tied to psychological factors or stress. However, many can still achieve an erection during self-stimulation.Presence of night-time (nocturnal) erections, but difficulty maintaining an erection during actual intercourse.
Natural Ways to Lower Cortisol
Managing cortisol levels naturally can improve both overall health and sexual function.
Here are effective, science-backed strategies:
Exercise regularly
Activities like walking, strength training, and yoga help reduce stress hormones. Even 15-30 minutes of outdoor activity daily can significantly lower cortisol levels.
Prioritize quality sleep
Getting 7-9 hours of sleep is essential for hormone balance. Proper rest supports testosterone recovery and reduces stress-related disruptions.
Follow a balanced diet
A Mediterranean-style diet is full of fruits, vegetables, whole grains, and healthy fats. It helps lower inflammation and supports healthy hormone levels.
Practice relaxation techniques
Methods such as deep breathing, muscle relaxation, and guided imagery can calm the nervous system. They also lower cortisol levels naturally.
Mindfulness and meditation
Regular practice helps reduce anxiety and controls cortisol levels. This boosts both mental and physical well-being.
Limit alcohol intake
Too much alcohol can drop testosterone levels. It can also hurt nerve function, making stress problems worse.
Consider natural adaptogens
Herbs like ashwagandha have been studied. They might lower cortisol levels and boost stress resilience. So, consult a doctor before using them.
Clinical Evidence: What Research Shows About Cortisol and ED
Research shows a clear link between cortisol levels and erectile dysfunction (ED). Stress hormones can affect sexual performance in different ways.

Normal response: cortisol decreases during arousal
In healthy people, cortisol levels usually decrease during sexual arousal. This drop helps the body maintain good blood flow and achieve an erection.In ED cases, this response is disrupted.
Studies show that men with ED often don’t see a natural drop in cortisol. This may affect their body’s sexual response.
Higher cortisol = lower erectile function
Clinical findings show that high cortisol levels relate to worse erectile performance. This means more stress hormones lead to poorer outcomes.Cortisol interferes with key mechanisms.
High cortisol can harm blood flow, nerve signals, and hormone balance. These are all key for getting and keeping an erection.
Chronic stress increases long-term risk.Prolonged stress and high cortisol levels can lower libido and increase the chances of ED.
Study 1: Cortisol-IIEF Correlation – Serum and Salivary Study (Nature, 2009)
A key study from the International Journal of Impotence Research (Nature, 2009) examined how cortisol in blood and saliva impacts erectile function. They used the International Index of Erectile Function (IIEF) for this analysis.
The study involved more than 105 men aged 30 to 72. Researchers measured both serum and salivary cortisol levels. They also assessed sexual performance scores.

Researchers found a strong negative link between bioavailable cortisol and salivary cortisol. They also noted a connection with IIEF scores. Higher cortisol levels are linked to poor erectile function, reduced sexual desire, and lower satisfaction.
Testosterone levels didn’t strongly link to erectile performance. This suggests that cortisol, a stress hormone, might be a better indicator of sexual dysfunction in some cases.
The study showed that active forms of cortisol, like bioavailable and salivary cortisol, affect sexual health more than total cortisol does.
High cortisol levels can block normal erectile function. This often happens because of stress and nervous system activation. This makes it a possible cause of ED.
Study 2: Healthy Men vs ED Patients – Cavernous Blood Cortisol (PMC 2023)
A key 2023 study in PMC (Translational Andrology & Urology) looked at cortisol levels during sexual arousal. It compared healthy men to those with erectile dysfunction (ED).
The study included 54 healthy men and 45 men with ED. Researchers measured cortisol levels in systemic and cavernous (penile) blood during various erection phases.
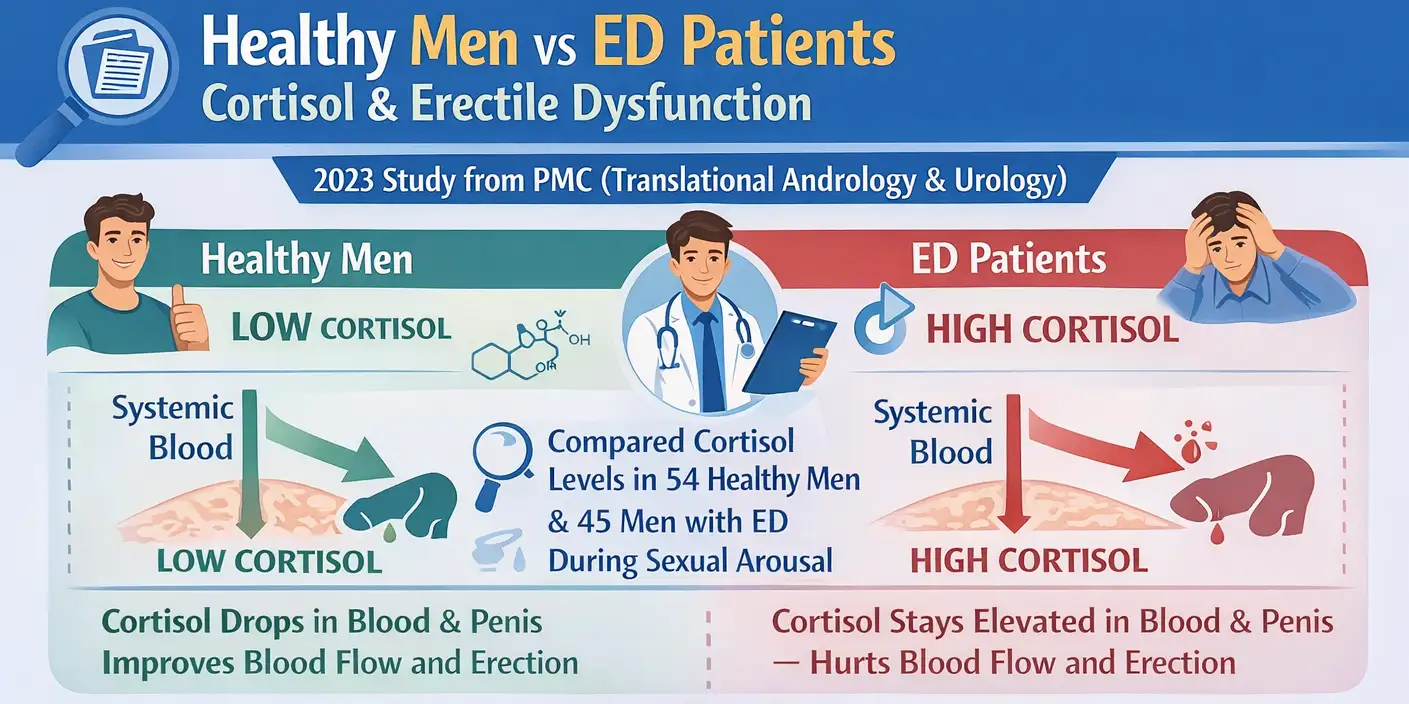
In healthy men, cortisol levels drop significantly when sexual arousal begins. This happens in the bloodstream and in the penile tissue. This drop appears to support normal erectile function.
In contrast, men with ED showed no meaningful decrease in cortisol levels during arousal. In some cases, cortisol even remained slightly elevated, indicating a disrupted stress response.
The findings show that lowering cortisol is key for a good erection. If cortisol doesn’t drop, it can hurt blood flow and affect sexual performance.
Researchers found that cortisol might inhibit the sexual response cycle. This means that high or unregulated cortisol can block normal erectile functions.
Study 3: Serum Cortisol and Erectile Function in the General Population (2024)
A 2024 study in the Archives of Urological Research looked at how serum cortisol levels affect erectile function in healthy men.
The study looked at men aged 45 to 60. It used blood tests to measure cortisol levels. The IIEF-5 questionnaire assessed erectile function.

Researchers found a positive link between cortisol levels and erectile function scores. This means men with normal erectile function had slightly higher cortisol levels than those with ED.
However, this relationship was not straightforward. Body weight (BMI) and waist circumference greatly affect cortisol levels and erectile performance. Higher values can lead to worse outcomes in both areas.
Men with ED often had more body fat and larger waists. This seemed to affect their hormonal balance more than cortisol did.
The study found that abdominal obesity was a better predictor of ED than cortisol levels. This was true even when considering factors like age, smoking, and alcohol use.
Study 4: Cushing’s Syndrome – Direct Hypercortisolism and Male Sexual Function
Cushing’s Syndrome is marked by high cortisol levels, known as hypercortisolism. This condition clearly shows how too much cortisol impacts sexual health.
High cortisol levels can lower libido and harm erectile function in men. This shows a direct link between hormones and sexual health.
In conditions like Cushing’s, high cortisol levels upset the balance of sex hormones. This often leads to lower testosterone production, which is key for sexual performance.
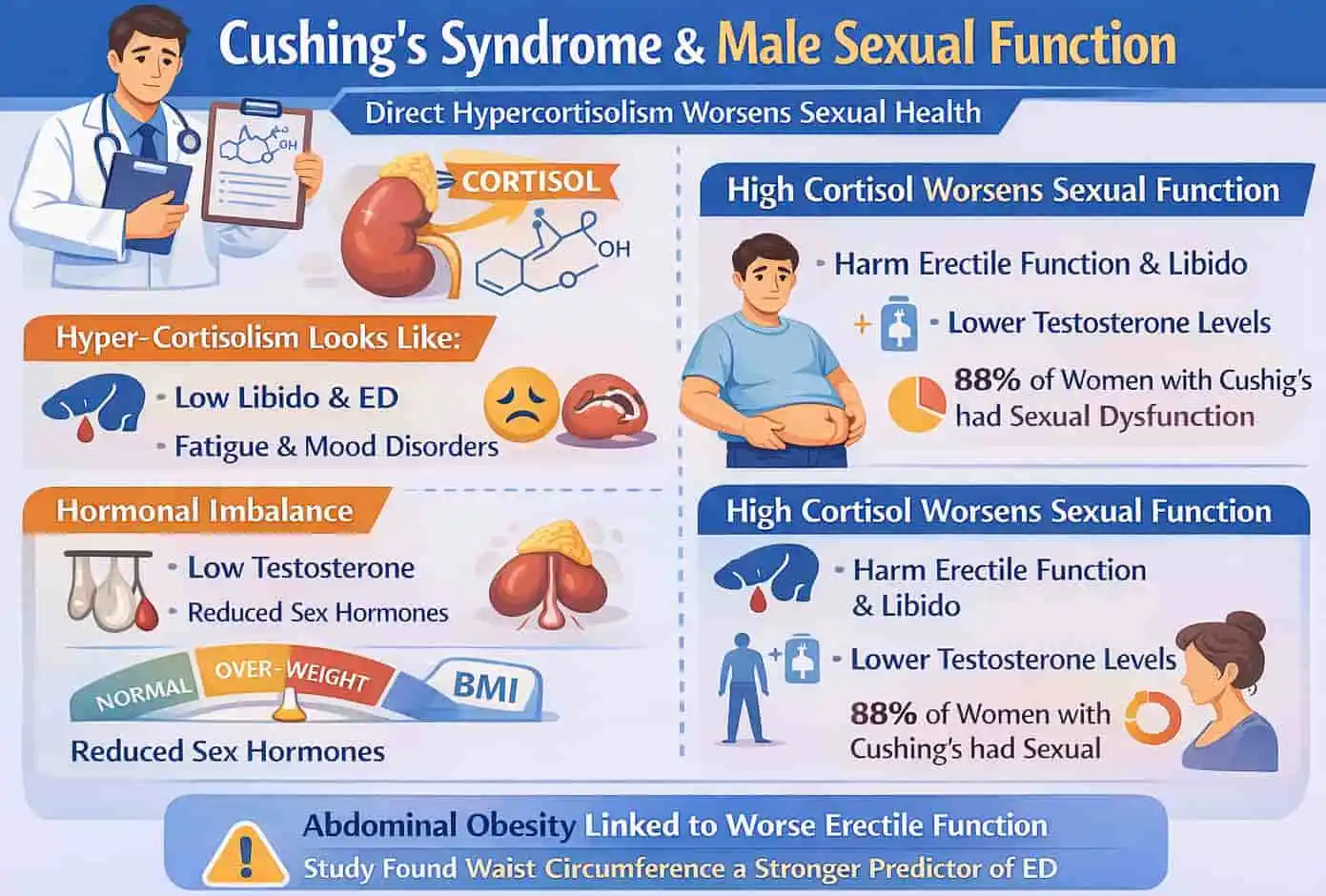
Studies in related groups, like women with Cushing’s Syndrome, showed that about 88% had sexual dysfunction. This issue is closely tied to high cortisol levels and low sex hormones.
High cortisol impacts the brain’s control centers, like the hypothalamus and pituitary. This disrupts hormonal signals that manage libido and erections.
Additionally, patients with Cushing’s often show symptoms like fatigue, mood disorders, and metabolic changes, which further contribute to sexual dysfunction.
Study 5: Hypothalamic-Pituitary-Adrenal Disease and ED Review (MDPI 2021)
A 2021 review in MDPI’s Journal of Clinical Medicine explored how HPA axis disorders impact erectile dysfunction (ED). It highlighted cortisol’s role and hormonal imbalances.
The review highlights that erection is a complex process. It needs good coordination between the brain, hormones, nerves, and blood vessels. Disruption in any of these systems can lead to ED.
Chronic activation of the HPA axis, from stress or illness, raises cortisol levels. This can harm sexual function by disrupting hormone balance and blood flow.
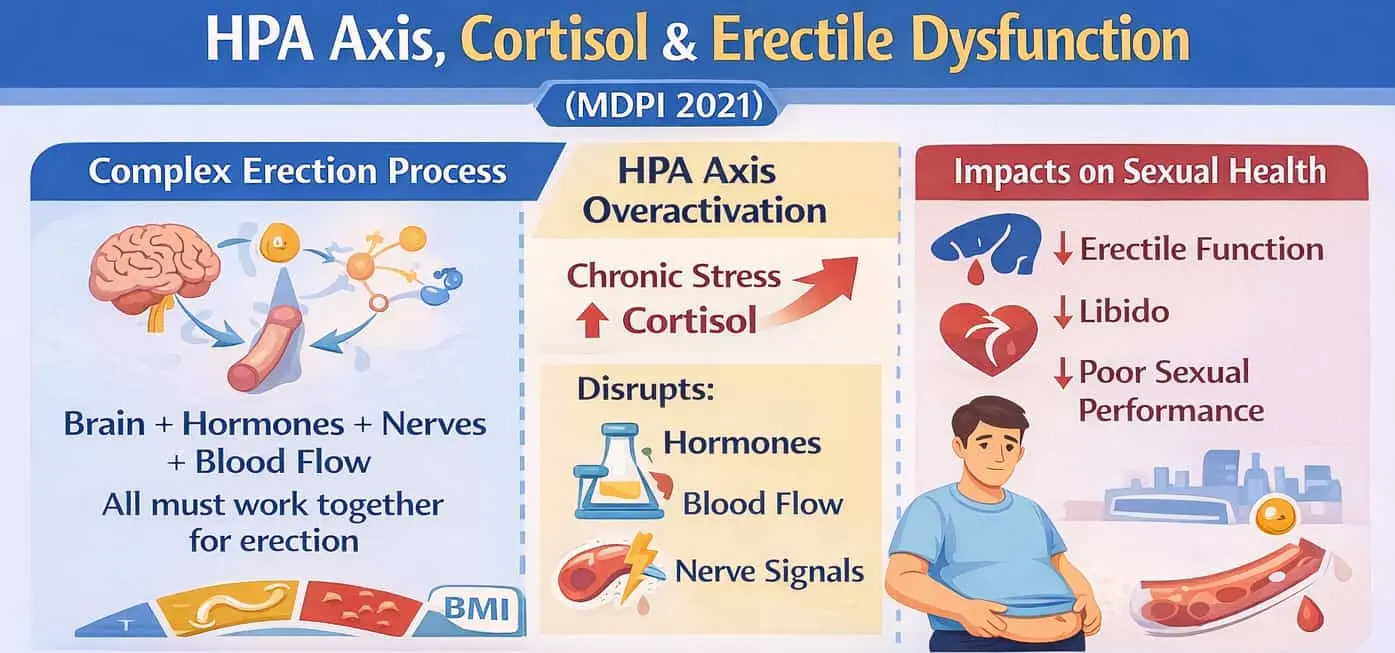
The study found that high cortisol levels relate to worse erectile function and lower sexual desire. This means more stress hormones are connected to poorer performance and less libido.
It also says that depression, diabetes, obesity, and alcoholism can cause “functional hypercortisolism.” This can raise the risk of ED by keeping the stress-response system active.
The review highlights that cortisol needs to drop naturally during sexual arousal. If this doesn’t happen, it can hurt erections by affecting blood flow and hormone signals.
The authors conclude that ED is usually caused by multiple factors. Cortisol imbalance works with things like metabolic health, cardiovascular function, and testosterone levels.
Study 6: Cortisol’s Inhibitory Role – Penile Tissue and Central Effect
A key study in Urological Research looked at how cortisol affects erections. It examined if this effect is direct at the penile tissue level or through brain mechanisms.
The study looked at cortisol levels in both blood types: systemic and cavernous (penile). It measured these levels during different stages of erection in healthy men. Cortisol levels went down as arousal went up. This suggests that lower cortisol is needed for normal erectile function.
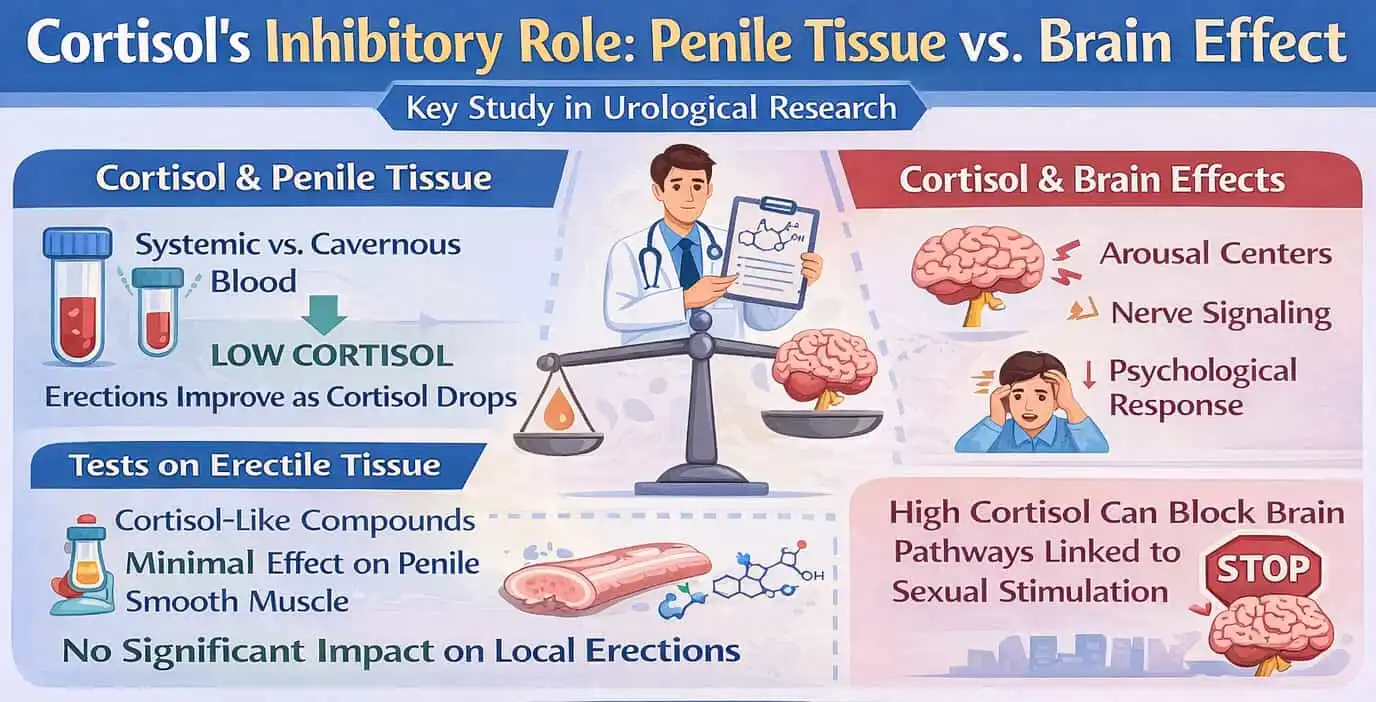
Tests on human erectile tissue showed that cortisol-like compounds had little effect on penile smooth muscle contraction. This differs from other chemicals that greatly affect erections.
This shows that cortisol doesn’t mainly work in the penile tissue. It means it doesn’t directly prevent erections through local blood flow.
Researchers found that cortisol mainly acts in the brain. It affects areas that control sexual arousal, nerve signaling, and psychological responses.
High cortisol might block the brain pathways linked to sexual stimulation. This can lower the signals needed to start and sustain an erection.
Medical Conditions That Link High Cortisol to Erectile Dysfunction
Cushing’s Syndrome – Clinical Hypercortisolism
Cushing’s Syndrome is a condition where the body makes too much cortisol for a long time. This can happen because of adrenal gland issues, pituitary tumors, or long-term steroid use. This condition clearly demonstrates how high cortisol can directly impact sexual health.
Excess cortisol causes hormonal disruption. It suppresses testosterone production, which leads to low libido and weaker erections.
Sixty-five percent of male patients say they have less libido and erectile dysfunction. They also see a big drop in testosterone levels, often over 50%. Research shows that treating conditions can help improve sexual function. Normal cortisol levels also play a key role. So, early diagnosis and management are key for recovery.
Chronic Psychological Stress – Functional Hypercortisolism
Chronic psychological stress is a key cause of functional hypercortisolism. In this case, cortisol levels stay high because of ongoing mental or emotional stress.
It’s not a medical issue like Cushing’s Syndrome. Research shows that men with long-term stress or anxiety have a 20-30% higher risk of erectile dysfunction. This is mainly because stress keeps the stress-response (HPA) axis active.
High cortisol levels can lower testosterone, affect blood flow, and disrupt sexual signaling. This leads to reduced libido and inconsistent erections.
When the body is in “stress mode,” it focuses on survival instead of reproduction. This can slowly harm sexual performance and upset hormonal balance.
Chronic psychological stress can cause erectile dysfunction due to cortisol. This can happen even without a medical issue like Cushing’s Syndrome.
Ongoing stress from work burnout, relationship issues, or money problems can keep the HPA axis active. This leads to a condition called functional hypercortisolism, or pseudo-Cushing’s.
High cortisol levels can lower testosterone. This may cause less interest in sex and trouble keeping erections.
Over time, even a few stress-related episodes can develop into performance anxiety, creating a cycle of psychogenic ED. Stress can mess with sleep. This raises cortisol and lowers testosterone, making things worse.
Diabetes Mellitus – HPA Axis Activation
Diabetes Mellitus is closely tied to erectile dysfunction. This happens through hormonal and vascular pathways. Chronic high blood sugar can trigger the HPA axis. This raises cortisol levels, which then disrupts hormonal balance even more.
High cortisol can lower testosterone, decrease libido, and weaken the body’s ability to get an erection.
Diabetes also harms blood vessels and nerves, which are crucial for keeping an erection. Together, these effects make ED more common and often more severe in men with diabetes.
Obesity – Metabolic Stress and Cortisol
besity leads to erectile dysfunction. It causes chronic metabolic stress, raising cortisol levels and throwing off hormonal balance.
Excess belly fat is tied to higher cortisol levels and lower testosterone. This can result in reduced libido and weaker erectile function.
Obesity also harms blood circulation and vascular health. This makes it harder to get and keep an erection. Together, these factors make obesity a significant risk factor for cortisol-related ED.
In 2024, a Swedish study revealed that waist circumference was the best predictor of ED, even after adjusting for cortisol.
Major Depression – Cortisol and ED
Major Depressive Disorder often leads to erectile dysfunction. This happens because it affects hormones and brain function. Depression can cause the HPA axis to stay active. This leads to high cortisol levels, which can lower testosterone and decrease sexual desire.
Changes in brain chemicals, like serotonin and dopamine, can lower arousal and pleasure. Fatigue and low mood also add to ED.
This combination of psychological and hormonal factors makes ED more common in men with depression.
Corticosteroid Medications – Exogenous Cortisol
Corticosteroids like prednisone can cause effects similar to too much cortisol. This leads to exogenous hypercortisolism.
These drugs help with inflammation, asthma, and autoimmune diseases. Using them for a long time can lower testosterone levels. This may reduce libido and lead to erectile dysfunction. They can also change blood flow, mood, and energy levels. This further affects sexual performance.
Careful medical supervision helps reduce side effects and keeps hormonal balance.
Long-term use of corticosteroids like prednisone, prednisolone, and dexamethasone is common. Doctors prescribe these for asthma, rheumatoid arthritis, inflammatory bowel disease, and autoimmune disorders.
Thereby suppressing the HPA axis, reducing testoestrone, and impairing nitric oxide production.
How to Lower Cortisol and Improve Erectile Function – Evidence-Based Strategies
Lifestyle Interventions – The Foundation
Making lifestyle changes helps manage cortisol levels and improve erectile function. Small, steady changes in stress, sleep, and daily habits can greatly improve hormone levels.
Regular physical activity is key. Moderate exercise, like walking, strength training, or yoga, lowers cortisol. It also boosts blood flow. Both are vital for healthy erections.
Quality sleep (7-9 hours) is vital. Deep sleep helps produce testosterone and regulate cortisol, which is key for sexual health.
Balanced nutrition: Eating whole foods, healthy fats, and antioxidants lowers inflammation and supports hormonal balance.
Stress Management Techniques:
Limit alcohol and avoid smoking. Both can harm hormones, blood vessels, and nerve function, making ED worse.
PDE5 Inhibitors – Restoring Blood Flow While Managing Cortisol
PDE5 inhibitors like sildenafil help treat erectile dysfunction. They work by boosting blood flow to the penis. They work by relaxing blood vessels. This boosts the effect of nitric oxide, which helps achieve and maintain an erection during sexual stimulation.
Tadalafil, sildenafil, and Vardenafil are the top options for treating erectile dysfunction. These medications don’t lower cortisol directly. They help fight one major issue: reduced blood flow and poor vascular response. These are especially useful for men facing stress and high cortisol levels, which can cause ED.
Tadalafil is suggested at a lower dose, which is Tadalista 20 mg, and is particularly useful for stress/psychological ED.
Sildenafil is found to be effective on demand for men with cortisol-mediated vascular ED.
You can easily buy all these medicines from Actiza Pharmacy if you have a valid prescription and proper consultation.
Medical Treatment for Underlying Conditions
For Cushing’s Syndrome, surgery is often the best option. It can remove the pituitary or adrenal tumor. Medicines can also help lower cortisol levels.
Testosterone replacement therapy is a choice for severe testosterone suppression due to cortisol. TRT, suggested under medical supervision, can help restore testosterone and improve sexual functionality.
Treating comorbidities such as diabetes, obesity, and depression can help lower HPA activation. This, in turn, reduces chronic cortisol levels.
Evidence-Based Supplements – Cortisol Reduction
Some supplements may help lower cortisol levels and boost erectile function. This is especially true for stress-related issues. These work by supporting hormonal balance, blood flow, and the body’s stress-response system.
Ashwagandha (KSM-66)
KSM-66 Ashwagandha is a strong adaptogen. It has been clinically studied and shown to lower cortisol levels by 15-28% compared to a placebo. It normalizes the HPA axis. This helps lessen cortisol’s negative impact on reproductive hormones and boosts testosterone production. Some studies show modest improvements in erectile function, especially for stress-related ED.
L-Arginine
An amino acid helps make nitric oxide. This is key for relaxing blood vessels and supporting healthy erectile function. It is especially helpful in mild to moderate vascular ED.
Zinc
Zinc plays a key role in testosterone production. Chronic stress can lower zinc levels. Supplementing with zinc might help restore hormonal balance and support sexual health.
Magnesium
Stress often lowers magnesium levels in the body. Taking magnesium can help balance the HPA axis. It may also improve sleep quality and lower cortisol levels. This can lead to better sexual function.
Testosterone Replacement Therapy
You can use Testosterone Replacement Therapy only if a blood test shows low testosterone levels. TRT can help restore sexual desire. It also improves erection quality and boosts energy levels. It’s not a first-line treatment. Always do it under medical supervision for safety and proper hormone balance.
Cognitive Behavioral Therapy (CBT)
Cognitive Behavioral Therapy (CBT) helps stop the cycle of stress, anxiety, and negative thoughts. These factors can lead to erectile dysfunction. It works well for psychogenic ED. This is when cortisol levels rise because of mental stress and performance pressure. By addressing these patterns, CBT helps improve confidence and reduce anxiety during intimacy.
Low-Intensity Shockwave Therapy
This non-invasive treatment stimulates new blood vessel growth (angiogenesis) in penile tissue. It naturally boosts blood flow. This is especially helpful for men with diabetes or vascular-related ED. Over time, it may enhance erectile function without the need for medication.
How to Know If Cortisol Is Driving Your ED – Diagnosis
To spot cortisol-related erectile dysfunction, check symptoms, review medical history, and run lab tests. Doctors may check stress levels, sleep patterns, and psychological factors. They also look for any underlying conditions. Blood tests measure cortisol and testosterone. Questionnaires and physical exams assess erectile function. If ED is inconsistent and linked to stress, along with signs like fatigue or anxiety, cortisol imbalance might be a factor.
Signs That High Cortisol May Be Driving Your ED
Erectile issues often get worse during stressful times. This can include work pressure, financial strain, or emotional anxiety. You find it hard to relax mentally or physically before or during intimacy.
Morning or nocturnal erections are still present, indicating that physical blood flow is likely normal.Erectile function seems to improve when you are relaxed, such as during vacations or low-stress periods.
You may have stress symptoms such as:
Doctors have diagnosed you with mental health conditions such as anxiety, depression, or PTSD. You are using long-term corticosteroid medications, which can elevate cortisol levels.
Blood tests show low testosterone without a clear physical cause, suggesting a hormonal imbalance. You have conditions that relate to stress-response activation. These include obesity, diabetes mellitus, and chronic alcohol use.
Diagnostic Tests to Discuss with Your Doctor
Doctors test for cortisol imbalance and its link to erectile dysfunction. They use hormonal tests and clinical assessments.

Morning Serum Cortisol (8 AM)
Measures baseline cortisol at its peak level. Abnormal values may indicate chronic stress or HPA axis imbalance.
24-Hour Urinary Free Cortisol
Evaluates total cortisol production over a full day. Considered a key test for detecting conditions like hypercortisolism and is useful in screening for Cushing’s Syndrome.
Late-Night Salivary Cortisol
Checks cortisol levels at night (when they should be very low). Elevated levels suggest disrupted circadian rhythm and HPA axis dysfunction.
Total and Free Testosterone
Assesses testosterone levels (normal range ~300-1000 ng/dL). Helps identify cortisol-related suppression of male hormones.
LH and FSH (Gonadotropins)
These hormones show how well the pituitary works. They help find out if low testosterone comes from primary or secondary causes.
IIEF-5 Questionnaire
A standardized scoring tool used to evaluate the severity of erectile dysfunction and track treatment progress.
DHEA-S (Dehydroepiandrosterone Sulfate)
An adrenal hormone precursor often decreases when cortisol levels are high or with adrenal dysfunction. This shows an imbalance.
Fasting Glucose / HbA1c
Screens for Diabetes Mellitus and metabolic stress, which are common conditions that can activate cortisol pathways and worsen ED.
Conclusion: The Truth About Cortisol and Erectile Dysfunction
Cortisol is important in erectile dysfunction, especially when stress is involved. Chronic high cortisol might not always be the main issue, but it can harm testosterone, blood flow, and mental focus. These are all key for healthy sexual function.
Conditions like Cushing’s Syndrome have a clear impact, but everyday stress can also lead to similar effects over time. To improve, focus on the root cause. Manage stress, restore hormonal balance, and adopt a healthy lifestyle for lasting results.
Key Clinical Summary: Cortisol and ED
Cortisol is the main stress hormone in the body. When its levels stay high for a long time, it can hurt erectile function. High cortisol suppresses testosterone production, leading to reduced libido and weaker erections.
It disrupts blood flow and the body’s response, both vital for getting and keeping an erection. Cortisol mainly acts through central (brain-mediated) mechanisms, affecting arousal, mood, and nerve signaling.
Cushing’s Syndrome shows a clear link between too much cortisol and sexual dysfunction. Chronic stress can create functional hypercortisolism, even without a medical disorder.
ED linked to cortisol is often inconsistent and stress-dependent, rather than constant. Effective management requires a combination of stress reduction, lifestyle changes, and targeted medical treatment.
Frequently Asked Questions – Cortisol and Erectile Dysfunction
Q1: Can stress alone cause erectile dysfunction without any physical problem?
Ans:- Chronic stress can cause psychogenic ED. It raises cortisol levels, which affects arousal, focus, and hormone balance. This can happen even if physical structures are normal.
Q2: Will Viagra or Cialis work if my ED is caused by high cortisol?
Ans:- Medications like sildenafil or tadalafil can still help by improving blood flow, but they do not address the root cause (high cortisol). Best results come when combined with stress management and lifestyle changes.
Q3: How quickly will erectile function improve if I reduce cortisol?
Ans:- Improvement can vary. However, many people see changes in a few weeks to a few months. This is especially true with better sleep, less stress, and healthy habits.
Q4: Can low cortisol also cause erectile dysfunction?
Ans:- Low cortisol isn’t often connected to ED, but severe hormone imbalances can still impact energy, mood, and sexual function.
Q5: Does ashwagandha really help with cortisol-related ED?
Ans:- Ashwagandha may lower cortisol and enhance stress response. This can help boost testosterone levels and improve sexual function, especially in cases linked to stress.
Q6: If I have Cushing’s Syndrome, will my erectile function recover after treatment?
Ans:- In many cases, yes. When cortisol levels go back to normal with treatment, sexual function often improves. This is especially true if treatment starts early.
Q7: Can I buy medicines for ED (sildenafil, tadalafil) from Actiza Pharmacy?
Ans:- Actiza Pharmacy is known as a manufacturer and exporter of generic medications. ED medicines should only be bought from licensed pharmacies or trusted suppliers. You need a valid prescription to ensure safety and authenticity.
